The Trojan Horse: How Bioengineered Bacteria Are Smuggling Viruses to Obliterate Tumors
Unlock the future of medicine: Bioengineered bacteria are being reprogrammed as Trojan horses to deliver viruses directly to tumors, bypassing immune defenses. Discover how this innovation, along with living skin gels and AI, is revolutionizing cancer therapy and regenerative medicine.
Written by Lavanya, Intern, Allegedly The News
COPENHAGEN, August 19, 2025
Cancer has long been a battlefield where conventional weapons like chemotherapy and radiation often cause immense collateral damage, wiping out healthy cells alongside the malignant ones. For decades, scientists have dreamed of a more precise, less destructive approach. That dream is now becoming a tangible reality, thanks to a remarkable convergence of synthetic biology and microbial engineering. Researchers are now reprogramming bacteria to act as Trojan horses, stealthily ferrying oncolytic viruses, viruses that specifically infect and kill cancer cells, deep into tumors while bypassing the body's vigilant immune system. This revolutionary approach isn't just an incremental improvement; it's a paradigm shift that could fundamentally reshape how we treat one of the world's most devastating diseases.
A New Frontline in Cancer Therapy: From Brute Force to Precision Strike,
Traditional cancer treatments operate on the principle of brute force. Chemotherapy and radiation therapy are designed to kill rapidly dividing cells, a characteristic of most cancer cells. However, this lack of specificity means they also harm healthy, fast-growing cells in the bone marrow, hair follicles, and digestive tract, leading to debilitating side effects like hair loss, nausea, and severe fatigue.
More recently, immunotherapy has emerged as a powerful tool, harnessing the patient's own immune system to fight cancer. While effective, it can be limited by the tumor's ability to evade detection or by a patient's pre-existing immunity to the therapeutic agent. For instance, a patient might have antibodies that neutralize an oncolytic virus before it can reach its target. This is a critical barrier that has historically hindered the full potential of viral therapies.
By contrast, the emerging microbial and viral approaches represent the ultimate in precision medicine. They leverage the unique biological properties of microbes to specifically target and destroy tumors, a strategy that has a long, albeit sporadic, history. The use of bacteria in cancer treatment dates back to the 19th century with Dr. William Coley's work, but it is only now, with the advent of modern genetic engineering and synthetic biology, that the true potential of this approach is being unlocked.
Engineered bacteria are becoming powerful allies in this fight. Certain bacteria, like a modified strain of Salmonella typhimurium, naturally gravitate towards the oxygen-deprived, nutrient-rich environment of solid tumors. This innate "tumor-homing" ability, which has been shown to result in bacterial accumulation in tumors at concentrations over 1000 times higher than in healthy tissue, makes them the perfect delivery vehicle. Instead of facing a systemic assault, the viruses are protected and transported directly to the tumor's core.
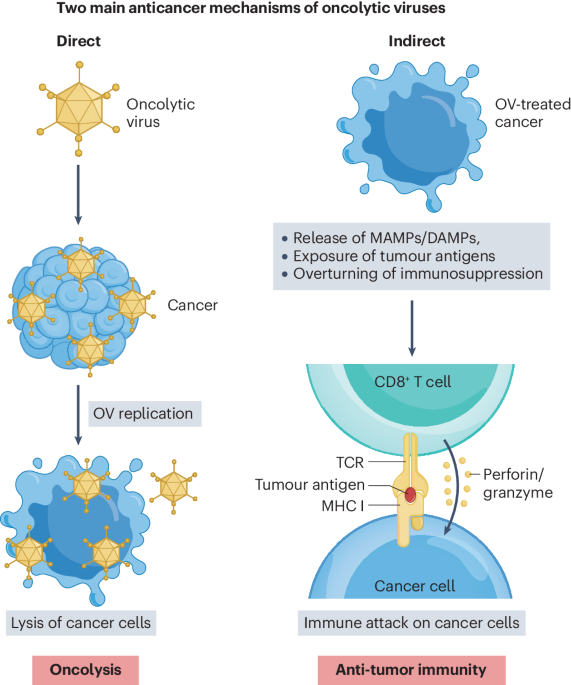
A recent breakthrough from Columbia University, published in Nature Biomedical Engineering, details a system called CAPPSID (Coordinated Activity of Prokaryote and Picornavirus for Safe Intracellular Delivery). This system is a prime example of microbial-viral collaboration. The engineered Salmonella strain acts as a biological shield, tucking the oncolytic virus inside its membrane, thus hiding it from the patient’s circulating antibodies. Once inside the tumor, the bacteria invade the cancer cells and lyse, or burst, releasing their viral payload directly into the tumor's interior. The oncolytic viruses then infect the cancer cells, replicate, and cause the cells to burst, releasing more viruses to infect neighboring cancer cells and further propagating the attack. This process is not only more targeted but also triggers a localized immune response that helps the body recognize and fight the cancer. The researchers also added a crucial safety feature: a genetic safeguard that ensures the virus can only replicate and spread in the presence of the bacteria, which are confined to the tumor, providing a failsafe against uncontrolled infection.
This approach is particularly promising for cancers with high mortality rates, such as liver, ovarian, and metastatic breast cancer. Clinical trials for similar bacterial delivery systems, like the non-toxic BacID developed by a team at the University of Massachusetts Amherst, are estimated to begin in the coming years, bringing this technology closer to patient access.
The Biggest Medical Innovations Reshaping Healthcare in 2025
Beyond the exciting frontiers of bacteria-powered cancer therapy, 2025 is proving to be a landmark year for medical innovation. The confluence of biology, engineering, and data science is giving rise to a new era of personalized and regenerative medicine.
- Genomics and Pharmacogenomics: The cost of whole-genome sequencing has plummeted, allowing for a truly preventative approach to healthcare. By analyzing an individual's genetic predisposition to diseases, doctors can create personalized health plans, including lifestyle modifications and targeted screenings. Pharmacogenomics is also transforming prescriptions by tailoring drug choice and dosage to a patient's unique genetic makeup, significantly reducing adverse drug reactions and improving treatment efficacy.
- AI in Diagnostics and Research: Artificial intelligence is no longer a futuristic concept; it's an indispensable tool in clinical practice. AI-powered tools are now being used to analyze medical images, detect subtle abnormalities in pathology slides, and predict disease progression with unprecedented accuracy. Startups like PathAI are leveraging deep learning to assist pathologists and radiologists, speeding up diagnosis and saving critical time. This has been particularly impactful in oncology, where AI models are being used to identify key biomarkers and guide treatment planning.
- Next-Generation Cellular Therapies: The success of CAR T-cell therapies for hematologic malignancies is expanding. Researchers are now tackling the challenge of using these therapies to treat solid tumors, which are notoriously difficult to penetrate. Innovations include developing "universal" off-the-shelf allogeneic therapies from donor cells, which are more scalable and cost-effective than personalized autologous treatments.
- mRNA Therapeutics: Building on the success of mRNA vaccines, the field is rapidly expanding into new frontiers. Researchers are exploring applications in treating metabolic and genetic diseases, cardiovascular conditions, and various forms of cancer, with the versatility of the technology making it a highly attractive avenue for drug development.
Bioengineered Skin: A New Frontier in Regenerative Care
While microbial engineering targets internal threats, a parallel revolution is underway in regenerative medicine, particularly in the field of wound healing and burn treatment. Bioengineered skin is on the verge of transforming burn treatment, cosmetic surgery, and trauma recovery by offering a superior alternative to traditional skin grafts.
Currently, the gold standard for treating severe burns is an autologous skin graft, which involves harvesting a piece of healthy skin from another part of the patient's body. This process is painful, creates a new wound site, and can be severely limited in cases of extensive burns.
Bioengineered skin circumvents these issues. For example, a research team at Tel Aviv University has developed a multi-layered, bioengineered skin graft that is more durable, flexible, and robust than previous attempts. Created from the patient's own cells on an FDA-approved nanofiber scaffold, this skin equivalent accelerates the healing process, with pre-clinical studies showing wound closure in half the time of standard therapies.
A different, but equally groundbreaking, approach is being pioneered by Swedish researchers. They've developed what they call “skin in a syringe,” a live-cell gel that can be applied directly to a wound or even 3D-printed into a custom graft. This unique gel, composed of living cells on tiny gelatin beads mixed with a hyaluronic acid gel, becomes liquid under pressure, allowing for easy application. Once on the wound, it solidifies, providing a perfect environment for the body to build new, functional dermis rather than scar tissue. This technology is also being used to create tiny, fluid-carrying channels from elastic hydrogel threads, a breakthrough that could solve the long-standing problem of creating vascularized organoids and artificial tissues for transplantation.
This work exemplifies how biotech startups and labs are leveraging synthetic biology to solve critical medical challenges. By designing and engineering biological systems with a purpose, they are creating living therapies that are more effective and safer than their chemical predecessors. Dr. David Mooney's work at the Wyss Institute at Harvard University is a testament to this, where his lab has developed implantable biomaterials that recruit and reprogram the immune system to destroy tumors or regenerate tissues, moving beyond traditional tissue engineering to a new paradigm of immunoengineering.
Analysis: The Symbiosis of Microbial Engineering and Regenerative Medicine
The twin advances in bacteria-powered cancer therapy and live-cell skin gels are powerful examples of biotechnology’s future impact. They demonstrate a move away from "one-size-fits-all" treatments towards highly personalized, living medicine.
- From a "Drug" to a "System": Instead of a static chemical compound, these new therapies are dynamic, living systems. The bacteria-virus system is an active delivery platform that intelligently navigates the body to a specific target. The live-cell gel is a biological scaffold that actively participates in the healing process, guiding the body to regenerate tissue.
- Addressing Fundamental Challenges: Both innovations address a fundamental bottleneck in their respective fields. For cancer, it's the problem of immune evasion and systemic toxicity. For wound healing, it's the challenge of limited donor skin and the inefficiency of current grafts. Synthetic biology provides a framework to solve these core issues by redesigning the biological components themselves.
- New Frontiers in Precision: These technologies open new frontiers in precision cancer therapies and regenerative care. By combining tumor-homing bacteria with a virus payload, scientists can create a bespoke treatment that is effective even in patients with pre-existing immunity to the virus. In regenerative care, 3D-printed grafts from a patient's own cells mean a perfectly matched, non-immunogenic solution for severe wounds.
Future Outlook: Clinical Applications and The Road Ahead
The clinical applications of live-cell skin gels in surgery and regenerative care are immense. Imagine a surgeon using a syringe to inject a live-cell gel into a deep wound, ensuring complete coverage and a faster, less painful recovery. Or a 3D printer creating a customized graft for a child with a severe burn, perfectly matching the contours of their body.
- Burn and Trauma Centers: Live-cell gels could become a standard treatment in trauma and burn centers, allowing for faster and more effective wound closure, reducing infection risk, and minimizing scarring. This could be particularly transformative for patients with extensive, third-degree burns who have very limited options for autografts.
- Cosmetic and Reconstructive Surgery: The ability to regenerate a patient’s own skin with minimal scarring could revolutionize reconstructive surgery, allowing surgeons to build new skin to repair defects from trauma or disease with perfect tissue matching.
- Chronic Wound Care: For patients with chronic conditions like diabetic ulcers, which often fail to heal, these gels could provide a long-awaited solution.
The work of pioneers like Dr. Sangeeta Bhatia at MIT, who applies micro- and nanotechnology to design miniaturized biomedical tools, including engineered probiotics for cancer detection and treatment, further highlights this trend. Her research underscores the power of a systems-level approach to medicine, where diagnostics and therapeutics are integrated into a single, intelligent platform.
What's Next for Patients and Physicians?
The next decade will see a dramatic acceleration in the development of living therapies. The bacteria-powered cancer therapy and bioengineered skin gels are not just isolated breakthroughs; they are proof-of-concept for a new way of thinking about medicine. We are moving from fixing a broken system to designing a better one. The ability to program biological systems, whether it’s a bacterium, a virus, or a skin cell, to perform specific tasks with unparalleled precision means we can now build therapies that are smarter, safer, and more effective. This isn't just a new chapter in medicine; it's an entirely new book.
The Grand Experiment: Your Questions Answered
- Given the complex, living nature of these new therapies, how will regulatory bodies like the FDA and EMA adapt their approval processes to ensure patient safety and efficacy in the long term?
- How will the cost and accessibility of these advanced, personalized treatments be managed to ensure equitable access to all patient populations, not just those with extensive financial resources?
- As we begin to use living, engineered organisms to treat diseases, what new bioethical considerations arise, and how can we establish a global framework for their responsible use and governance?
Sources
Nature Biomedical Engineering, Molecular Therapy, Columbia University, University of Massachusetts Amherst, Wyss Institute at Harvard University, Tel Aviv University.




